- Support: 24/7 Emergency Call
- Email Us: care@jeevanrakshakhospital.com
Robotic vs Traditional Joint Replacement: What Patients Should Know
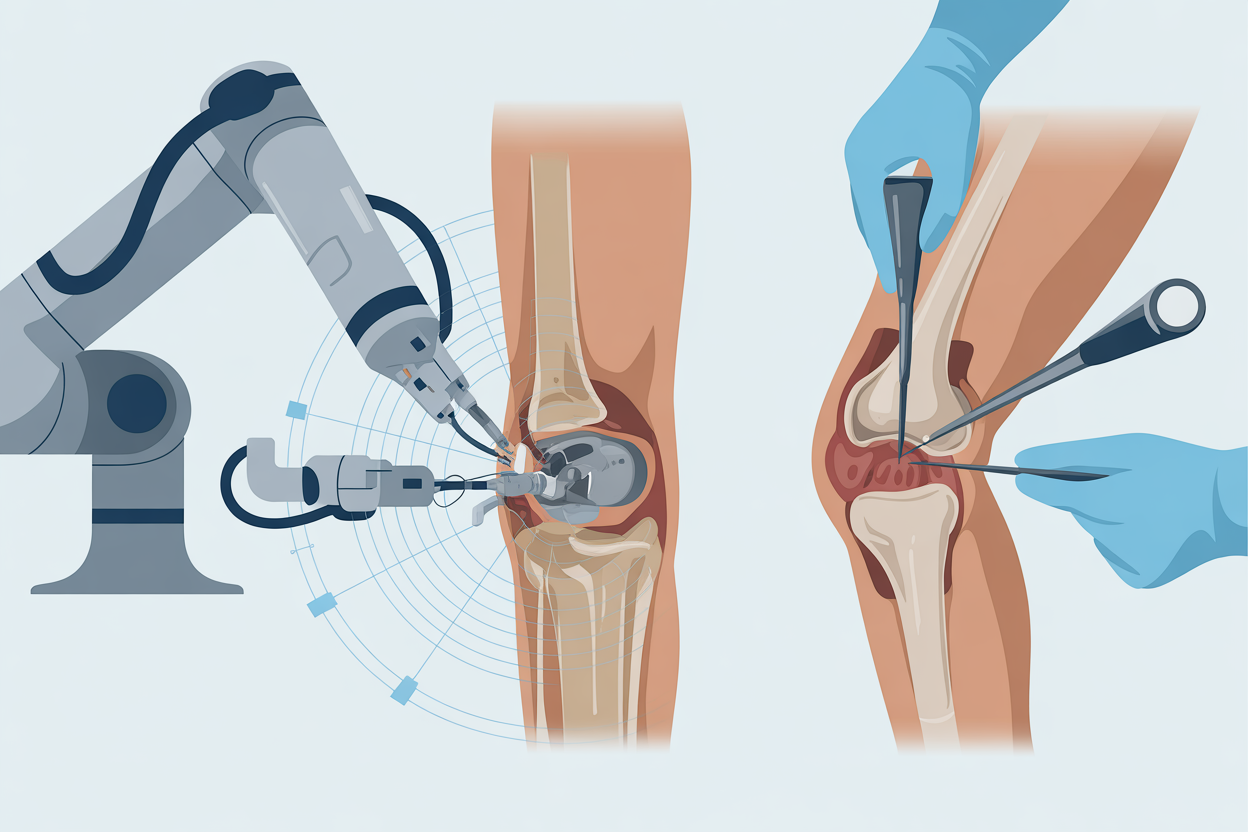
Joint replacement surgery has transformed the lives of millions suffering from chronic knee or hip pain. Today, patients facing this procedure have an important decision to make: robotic-assisted surgery or traditional techniques. Understanding the differences between these approaches can help you make an informed choice that’s right for your health and lifestyle.
What Is Robotic Joint Replacement?
Robotic-assisted joint replacement doesn’t mean a robot performs your surgery. Instead, your surgeon uses an advanced robotic system as a precision tool to plan and execute the procedure. Before surgery, detailed 3D imaging (CT or MRI scans) creates a custom map of your knee or hip anatomy. During the operation, the robotic system guides your surgeon to make cuts and position implants with submillimeter accuracy.
The surgeon maintains complete control throughout the procedure, but the robot enhances precision and allows real-time adjustments based on your unique anatomy. This technology uses AI-based 3D mapping and real-time navigation to achieve alignment accuracy under 1mm.
How Traditional Joint Replacement Works
Traditional joint replacement relies on the surgeon’s experience, skill, and manual technique. Surgeons use standard guides and instruments to remove damaged bone and cartilage, then position the artificial joint. This time-tested approach has decades of proven success and remains widely available across hospitals.
While traditional surgery depends more on manual estimation, experienced surgeons achieve excellent results using established protocols and mechanical alignment guides.
Key Differences Between the Two Approaches
| Feature | Traditional Surgery | Robotic Surgery |
|---|---|---|
| Alignment Accuracy | Good but variable | Submillimeter precision (<1mm) |
| Incision Size | 6–8 inches | 4–6 inches |
| Operative Time | Shorter | Longer (learning curve involved) |
| Cost | Lower | Higher upfront cost |
| Technology | Manual guided technique | AI-based 3D mapping |
| Customization | Standard guides | Personalized to anatomy |
Advantages of Robotic Joint Replacement
Superior Precision and Alignment
Robotic systems achieve extreme accuracy in implant positioning, which translates to better stability, smoother movement, and potentially longer implant life. Studies show robotic-assisted procedures reduce alignment outliers by approximately 10-24% compared to conventional methods.
Faster Recovery
Less soft tissue damage during surgery means reduced swelling, less post-operative pain, and quicker rehabilitation. Many patients report faster return to daily activities compared to traditional knee replacement.
Reduced Complications
Robotic-assisted hip replacement shows significantly lower intraoperative complication rates compared to conventional surgery. For knee replacement, robotic procedures reduce major complication rates by 50-70%, with infection rates below 0.5%.
Longer Implant Lifespan
Better alignment means robotic implants often last 20+ years, reducing the need for revision surgeries. This is especially beneficial for younger, active patients.
Minimally Invasive Approach
Smaller incisions lead to less blood loss, reduced scarring, lower infection risk, and better cosmetic results.
Advantages of Traditional Joint Replacement
Proven Track Record
Traditional surgery has decades of clinical success and extensive long-term outcome data. Surgeons worldwide have performed millions of these procedures with excellent results.
Lower Cost
Traditional joint replacement is more affordable upfront, making it accessible to more patients. This matters when budget is a major constraint.
Shorter Operative Time
Conventional procedures typically take less time in the operating room, which reduces anesthesia exposure and associated risks.
Wide Availability
Traditional techniques are available at virtually all hospitals and don’t require specialized robotic equipment.
Potential Drawbacks to Consider
Robotic Surgery Limitations
Higher initial cost: Advanced technology increases upfront expenses, though long-term savings from fewer revisions may offset this
Longer surgery time: Robotic procedures take more time, especially during the surgeon’s learning curve, which can increase infection risk
Rare technical complications: Pin-hole fractures, pin-related infections, and occasional equipment-related issues have been reported
Limited long-term data: While promising, robotic systems are newer with less decades-long outcome data
Traditional Surgery Limitations
Variable alignment accuracy: Results depend more heavily on surgeon experience and manual technique
Larger incisions: More tissue trauma can mean longer recovery and more visible scarring
Less customization: Standard guides may not perfectly match every patient’s unique anatomy
Who Should Consider Robotic Surgery?
Robotic-assisted joint replacement may be ideal for:
Younger, active patients wanting maximum implant longevity
Those with unusual anatomy or complex deformities requiring customization
Patients prioritizing faster recovery and minimal scarring
Individuals willing to invest in advanced technology for potential long-term benefits
Who Might Choose Traditional Surgery?
Traditional joint replacement remains an excellent choice for:
Patients with budget constraints
Those with mild to moderate arthritis and minimal deformity
People who prefer time-tested, widely available approaches
Anyone uncomfortable with newer robotic technologies
Making Your Decision
Both robotic and traditional joint replacement can deliver excellent outcomes when performed by skilled surgeons. Current research shows similar functional scores and patient satisfaction between the two approaches, though robotic systems offer advantages in precision, component positioning, and reduced complications.
The best choice depends on your individual anatomy, activity level, budget, recovery goals, and surgeon expertise. Consult with an experienced orthopaedic surgeon who can assess your specific condition and discuss which approach aligns with your needs.
Remember: surgeon experience matters more than technology alone. Whether you choose robotic or traditional surgery, selecting a qualified specialist with extensive joint replacement experience is crucial for optimal results.
